|
The cells in that dish aren’t the same as the cells in living tissues affected by SARS-CoV-2. 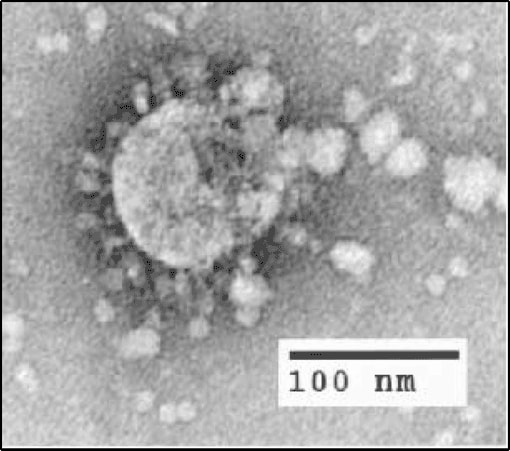
Compared with a lab dish, living people are complicated. As researchers learn more and more about the novel coronavirus that causes COVID-19, this knowledge - gathered through unmatched levels of scientific cooperation - is being turned against the virus in real time. Here’s a primer on viruses in general and SARS-CoV-2 in particular. Today, as COVID-19 spreads around the globe, the greatest army of medical scientists ever assembled is bent on learning all it can, as fast as it can, about SARS-CoV-2, the virus behind the pandemic. Respiratory syncytial virus, which typically causes colds, can do both: In adults, it destroys cilia in children, it can kill the cells, which can be deadly.“Know your enemy,” Sun Tzu, the great sage of war, wrote some 2,500 years ago. Other pathogens - like influenza - can kill ciliated cells. Some pathogens, like the coronavirus, just damage cilia, leaving the cells they protrude from intact. Other viruses and bacteria can also damage the body’s ability to use mucus to trap and remove foreign invaders, Chakrabarti says. 
The colored lines show how fast the beads are moving, with blue indicating slower speeds and red noting faster speeds. Here microscopic beads move around the surface of uninfected lab-grown cells first and then around infected cells, illustrating mucus movement. But coronavirus-infected cells lose those cilia and no longer push mucus, eliminating a barrier that would normally help prevent the virus from invading the lungs. Normally, cilia move in synchronized waves to push mucus away from the lungs, toward the throat where foreign objects are swallowed. When the team added microscopic beads to the surface of infected cells to measure mucus movement, those beads largely stayed still - a sign that the cells wouldn’t move mucus through the respiratory tract and into the throat to be swallowed. Images showed short, stubby cilia on the surface of the infected cells rather than the long projections found on healthy cells. Understanding how the coronavirus invades different parts of the body can help researchers find ways to block it.Ĭhakrabarti and colleagues infected lab-grown human cells that mimic the lining of the respiratory tract with the coronavirus. That lack of cilia could help the virus invade the lungs and cause severe COVID-19, says Lisa Chakrabarti, a viral immunologist at the Pasteur Institute in Paris ( SN: 6/11/20). Sign up for e-mail updates on the latest coronavirus news and research 
When it infects respiratory tract cells, the virus appears to clear tracts of cilia, and without the hairlike structures, the cells stop moving mucus, researchers report July 16 in Nature Communications. To protect the lungs, objects that don’t belong - including viral invaders like the coronavirus - get stuck in mucus, which is then swallowed ( SN: 9/15/20).īut the coronavirus throws that system out of whack. Normally, those cilia move in synchronized waves to push mucus out of the airway and into the throat. A coronavirus infection can mow down the forests of hairlike cilia that coat our airways, destroying a crucial barrier to keeping the virus from lodging deep in the lungs.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
